March 25, 2026
post
Unpacking Practice Readiness
Lessons Learned from the Big 10 Practice-Ready Nursing Initiative

In the age of competency-based education and the recent updates to clinical competencies in nursing, the role of nursing continues to expand, and ensuring new graduate nurses are practice ready is a significant focus for academic institutions.
Defining and assessing practice readiness remains a challenge. Employers and new graduates report gaps or anxiety in multi-patient prioritization, communication, and applying clinical judgment in high acuity or complex situations.
To better prepare nursing students for the realities of clinical practice, leaders across the Big10 collaborated to develop the Big10 Practice Ready Nursing Initiative.
Key Topics from the Webinar
The shift toward competency-based education has placed increasing pressure on academic institutions to demonstrate outcomes and align with employer expectations on the definition and assessment of practice readiness.
VR simulation supports scalable, cost-effective simulation: Increasing simulation alone is not always feasible – traditional simulation can be costly, time and resource-intensive, and may require significant coordination to acquire space. IVR simulations both increase presence and immersion in ways that traditional simulation does not, while supporting scalable, repeatable simulations that can be completed independently or within groups.
Leverage data and analytics to inform decision-making: Analytics and data offer objective, evidence-based feedback to students and provide data-driven insights for educators to be able to make informed decisions about curricula, coursework, or remediation.
Embed VR simulation within structured frameworks: Importantly, virtual reality clinical simulations are not a standalone resource – rather, VR simulation is part of a larger ecosystem of modalities that drive learning through immersive simulation in a psychologically safe space that allows students to reflect on strengths and identify mistakes, taking those insights to a structured debriefing with a trained facilitator to maximize learning.
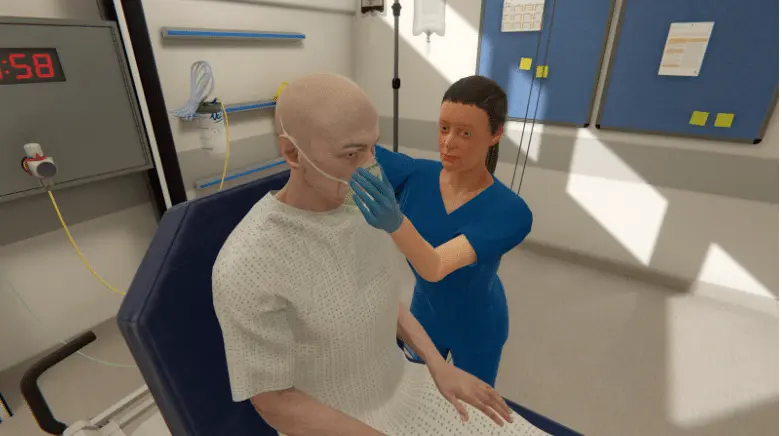
How Leaders Across the Big10 Created the Practice Ready Nursing Initiative
This multi-site collaboration was led by:
Cynthia Bradley, PhD, RN,CNE, CHSE, ANEF – Associate Professor and Director of Simulation, University of Minnesota School of Nursing
Michelle Aebersold PhD, RN, CHSE, FSSH, FAAN – Clinical Professor and Vice Chair for Research Systems, Populations and Leadership, University of Michigan School of Nursing
Ann Loomis, PhD, RN, CNEcl – Clinical Associate Professor, Purdue University School of Nursing
The leaders of the Big10 selected virtual reality simulations due to the power of immersive learning experiences, as increased presence can improve knowledge retention.
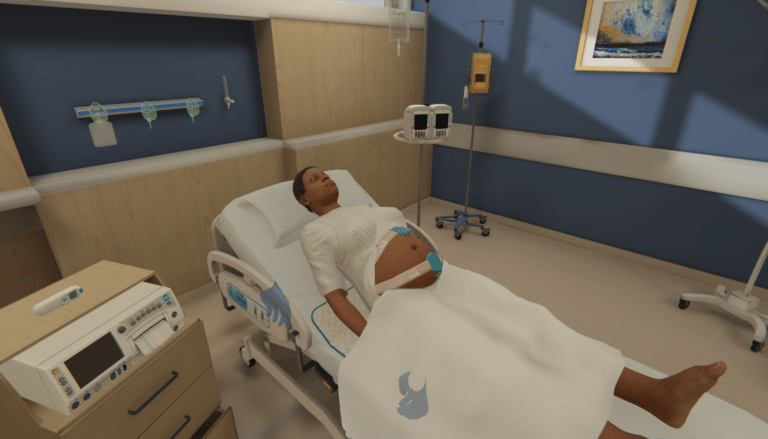
In partnership with OMS, leaders from the Big10 developed Multi-Patient immersive virtual reality simulations (IVRS) to support the development and assessment of clinical readiness and decision-making for nursing students preparing for the transition to practice.
These simulations were implemented across sites and cohorts and focused on the cognitive skill development required to competently and efficiently manage a caseload with multiple patients. The skills focused on in this study were: Clinical judgment, clinical decision-making, prioritization, and delegation.
Students began with one simulation, managing care for one virtual patient, and worked through the remaining four scenarios, adding another patient in each scenario until students were autonomously managing care for five virtual patients.
This scaffolded learning provided a more open and complex environment as scenarios went on, reflecting both the cognitive load of bedside nursing and the prioritization and delegation skills required to navigate workflow disruptions and analysis of new information.

The Role of Data and Debriefing
These immersive VR simulations were thoughtfully integrated into the nursing curriculum to accommodate the scale needed to support large cohorts of students in simulation.
VR simulations were embedded into the curriculum alongside orientation, prebriefing, and structured debriefing to set expectations, familiarize students with the technology, and facilitate reflection and discussion from immersive learning experiences.
Competency assessment tools were developed by the team, resulting in the CCEI-VR, and used to assess core components of readiness.
Additionally, the Big10 team used analytics from the OMS platform to track trends, individual progress, and identify gaps across cohort-level data. Analytics such as actions taken or missed, timestamps, and evidence-based feedback were also identified as key metrics to identify patterns and support the assessment of practice readiness.
The Future Implications
Thoughtful integration of virtual reality simulations can support students and faculty in bridging theory to practice, supporting the development and assessment of practice readiness across nursing programs.
This initiative reflects a broader shift in nursing education from time-based preparation to performance-based readiness.
To learn more about the Big10 Practice Ready Nursing Initiative and the insights gained from this research, watch the full webinar on the OMS YouTube channel.
Related
Ready to get real?
See how OMS can help your organization build confidence, competence, and clinical readiness for today’s healthcare.