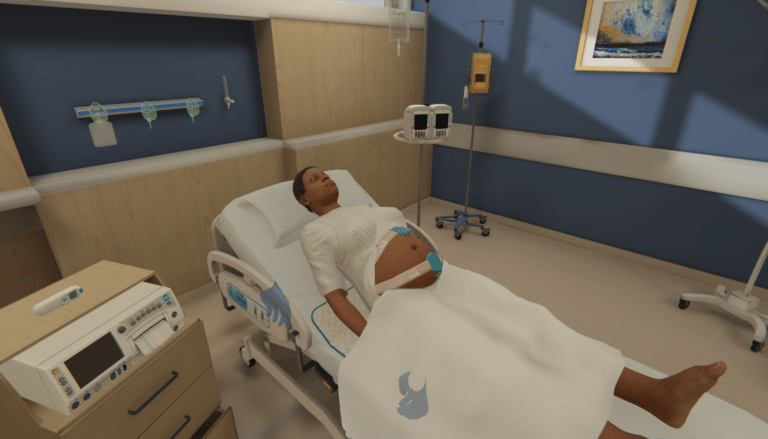
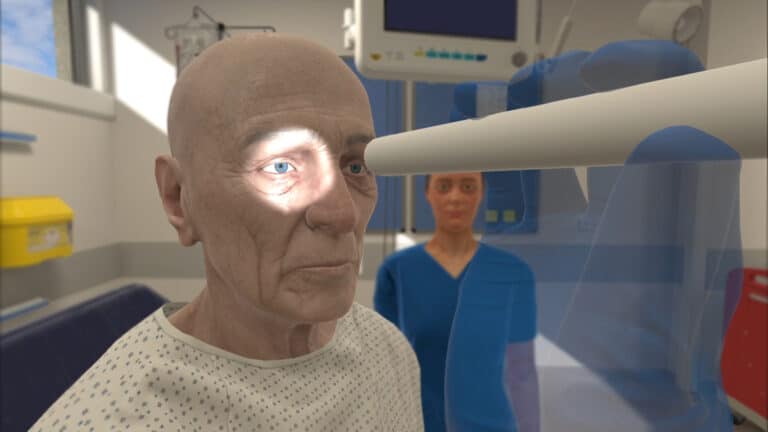
Virtual Reality: A New Wave for Simulation-Based Education
Whether in the classroom or the clinical setting, opportunities for learners to practice skills freely and in a safe environment are limited. However, replicating real-world clinical scenarios is crucial in preparing students for practice and reinforcing knowledge and skills for clinicians. This recreation of specific clinical situations is often referred to as ‘simulation-based education’, and…