Oxford Medical Simulation Secures £5 Million Growth Financing from Salica Investments to Accelerate Expansion of Immersive Clinical Training
Funding to support US health system and academic growth and accelerated product innovation.

Funding to support US health system and academic growth and accelerated product innovation.

With the evolving landscape of clinical practice, it’s also imperative that nurses are afforded the opportunity to build new skills like utilizing advancing technology or implementing new clinical treatment methods.

The National League for Nursing (NLN) conference this year brought over 1,000 nurse educators, leaders, simulation experts to sunny Orlando, Florida for a week of connection, networking, and learning about the state of nursing education today and how we can continue to improve, enhance, and drive better patient outcomes through healthcare training. The OMS team…

Each year, nurses are required to complete competency assessments or take part in programs that confirm their ongoing knowledge and skill development in patient care. Policies and standards, like those outlined by the Joint Commission, ANCC Magnet, or the Nursing & Midwifery Council, are meant to play a critical role in ensuring patient safety and…
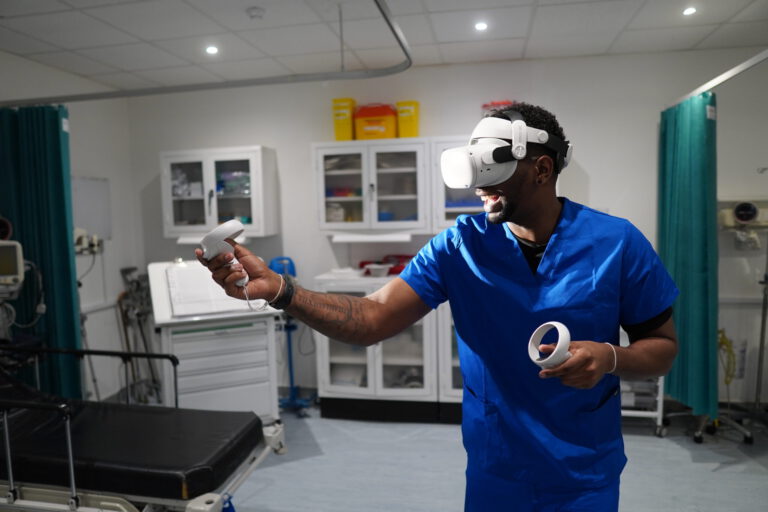
Putting on a virtual reality headset and diving into an interactive game or experience, like riding a roller coaster, can be a great way to enjoy the virtual world, but those types of simulations can also result in VR motion sickness, sometimes called ‘cybersickness’. Motion sickness is not a new concept, but it may be…

At OMS, we have always been committed to creating the most realistic learning experiences for our clients and learners. With advancements in AI technology and the growing accessibility of VR headsets, we are excited to introduce a new generation of OMS scenarios! As learners evolve and develop their skills, their needs change. They may need…
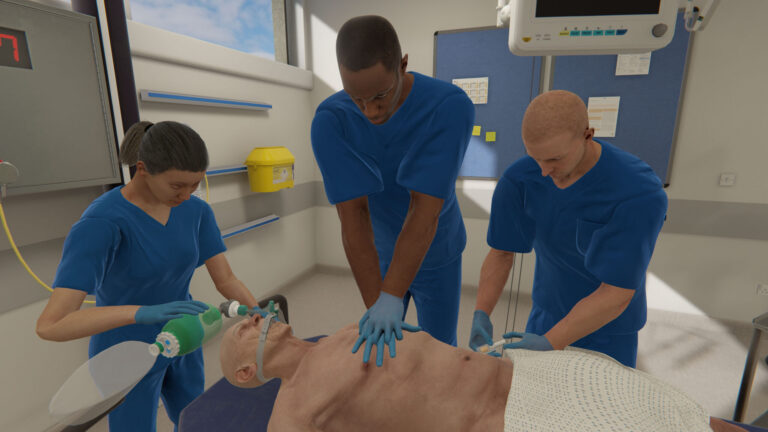
Acuity levels often refer to a patient’s status level, with higher acuity meaning a more unstable condition. Sepsis is one example of a condition with high acuity. A high acuity setting may refer to the intensive care unit (ICU) or emergency department (ED). Nursing in high acuity environments requires honed critical thinking and clinical reasoning…

When it comes to healthcare training and education, simulation is a core component designed to apply, test, and refine clinical skills in a safe environment for the learner. There are many ways to accomplish this, from traditional methods like manikin-based simulations and the use of standardized patients to more modern methods like virtual simulation and…
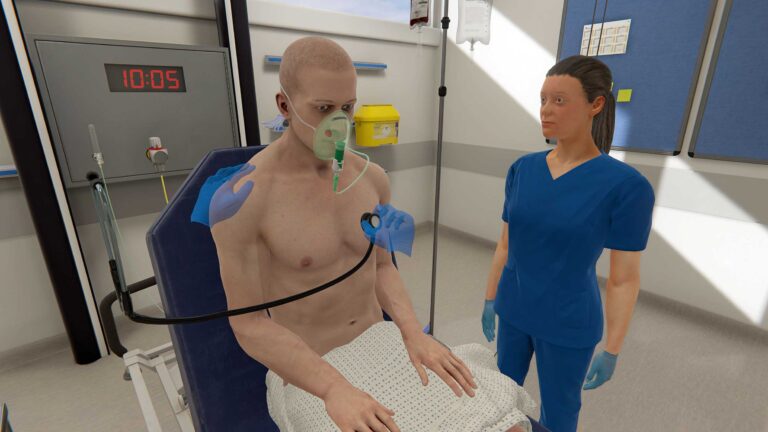
What’s the deal with virtual reality? And why is it making such big waves? Maybe it’s time to pick up surfing and come along for the ride…but how do you know it’s the right way to go? Start at the beginning – read on for the core benefits of using VR in nursing education: Psychological…

In September of this year, we hosted a group of leaders from across the United States, inviting them to join us in San Antonio for a roundtable discussion on bridging the gap between nursing school and the transition to practice. Understanding the difficult nature of transitioning from schooling to practice, it was imperative for us…
End of content
End of content
Be the first to know what’s next. Sign up for our newsletter.

Oxford Medical Simulation Inc., 240 Elm Street, 2nd and 3rd Floor, Somerville, MA 02144
Oxford Medical Simulation Ltd. Registered in England and Wales (Company No. 10587122) // Registered office: 201 Borough High Street, London, England, SE1 1JA
Oxford Medical Simulation Limited is committed to achieving Net Zero emissions by 2035 for emissions scopes 1, 2 and 3. The commitment was made on 24 March 2025 by the company’s board of directors.