When you think about using virtual simulation, you likely think about scenarios that learners go through to reinforce important concepts and to practice clinical skills.
In many cases, you’re exactly right. Virtual reality has been used for some time in healthcare settings, particularly in education.
As VR continues to grow, there are more and more possibilities for how it can be used, not just for skill-building and maintenance, but also as a tool for assessment.
What makes VR a good candidate for assessment?
Currently, VR simulations typically involve having a learner first orient to the equipment and context of the case, prepare as instructed, and take on the role of practitioner and run through the scenario.
Then, learners may receive feedback and get time to reflect, and in many cases, come together with a group of their peers and a facilitator to debrief on the case.
With skill-building, repetition is key – which is one big difference between physical and virtual simulations. In VR, learners can repeat the scenario as many times as they need to feel comfortable and confident in their clinical skills, before ever being evaluated.
Scenarios like those that OMS creates are based in best practices and current evidence. These VR simulations are standardized, and because of their consistency, there’s no need to worry about variability between raters.
Often in assessments, faculty are responsible for observing, taking notes, ensuring equipment or actors provide the right responses, and grading during an assessment. They are frequently expected to provide feedback and justification for the grade.
The objective nature of VR simulations, along with the automated, evidence-based feedback, frees up faculty from multitasking during evaluations and provides clear data and recommendations to the learner to improve their future performance.

With VR, faculty can put their focus on the learner and let OMS do the rest – there are no worries about responses varying from one learner to the next, and faculty can instead be fully present in observing the learner, using their expertise to provide pointed feedback.
For these reasons, among others, institutions are already seeing the benefits of implementing VR as a tool for assessment.
How is it being used for assessment?
How it’s used depends largely on the facility, the learner level, and the key concepts and objectives being met.
In other areas of healthcare, like emergency medicine, VR simulations have been used to assess clinical competence.
Authors reported VR as a good tool in assessing both procedural skill and non-technical skills like communication, history taking, and clinical decision making.
They also reinforced the notion that in using VR, educators have a reduced cognitive load, particularly for case authoring.
With a reduced likelihood of bias, as well as standardized scenarios with automated, evidence-based feedback, it’s no wonder why VR is arising as a valuable assessment tool for a wide range of clinical skills, both procedural and non-technical.
Whats to come...
As VR continues to expand the possibilities for educators and trainers, there’s so much more to come from its use as an assessment tool.
You can use it to capture data that aligns directly with competency frameworks, like the NCLEX.
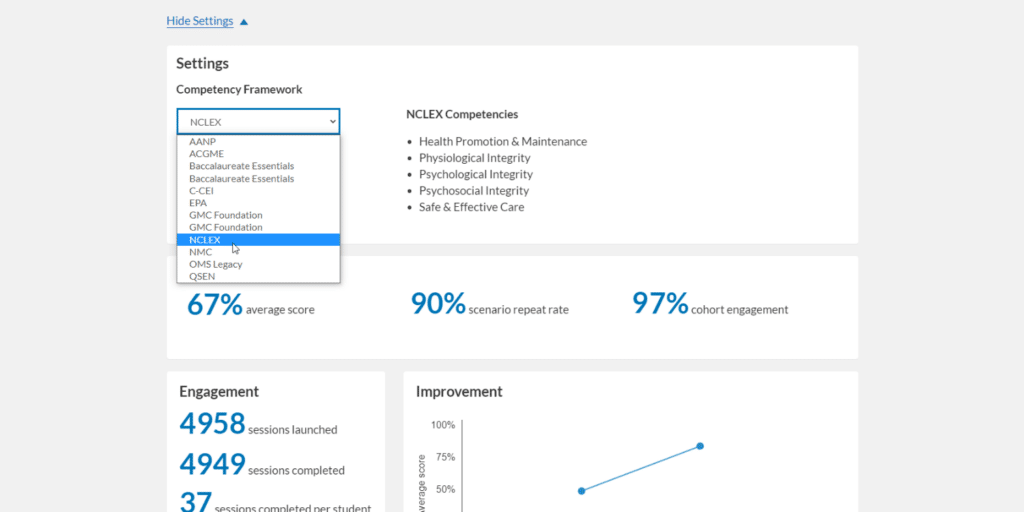
As it can be difficult to write test questions that require multiple points of knowledge to answer, you’ll likely find you can use VR to assess higher-level thinking skills, like clinical reasoning and decision making.
Learners are required to make effective decisions in real time, more closely resembling the realities of clinical practice.
And because this all remains virtual, there is no fear of endangering others, which provides a layer of psychological safety, even in evaluation.
With OMS, learners may have access to these simulations in their own time, meaning they can repeat these scenarios as many times as they need, without the need for faculty presence or supervision.
To learn more about how you can use OMS as a learning and assessment tool, set up a time to chat with us here.