Virtual Reality
-
-
The True Cost of Nursing Turnover: Why Nurses are Resigning and What It Means for the Healthcare Industry
Nursing has seen a shift in recent years that has caused alarm – higher turnover rates, staff shortages, and an increased demand for healthcare professionals have impacted the remaining staff and patients. It’s significantly financially costly for hospitals to replace lost staff, not to mention the time and resources cost of finding a suitable replacement….
-
Oxford Medical Simulation Raises $12.6 Million in Series A Funding to Address Critical Healthcare Training Gap with Virtual Reality
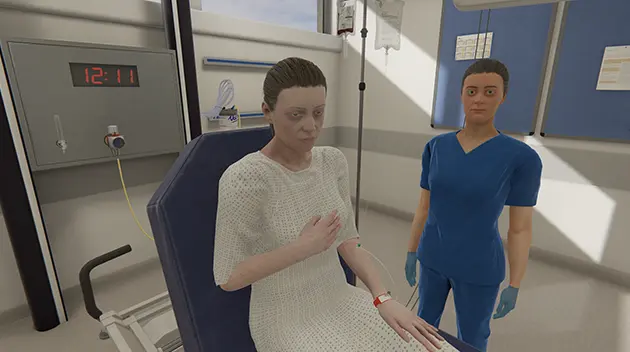
Talking with a patient is one of the best ways for healthcare professionals to hone their communication skills – gathering history, explaining rationale, building rapport, or even having difficult conversations.
-
Changing the Face of Education: Virtual Reality in Curriculum
In healthcare education, students often must retain a hefty amount of information, and on top of that, they must build psychomotor skills they can take with them into clinical practice.
Simulation is a well-known method to begin bridging the gap between knowledge and practice, and while it certainly has a place in healthcare curricula, it also has its limitations.
-
Healthcare Simulation | Interprofessional VR Simulation | Uncategorized | Virtual Reality Medical Training
OMS for Interprofessional Team Building
Building a safe space for a working environment is imperative to interdisciplinary team success in healthcare settings. VR can be used as a way to connect the interprofessional team from any space, providing similar benefits to that of in-person team building simulations.
-
OMS Partner with The Big 10 on Multi-Patient VR Simulation
Big 10 Practice-Ready Nursing Initiative is a partnership between the University of Minnesota School of Nursing, University of Michigan School of Nursing and Purdue University School of Nursing. The initiative was formed to respond to the issues arising from nurse graduates being unprepared to practice in today’s highly complex and dynamic care environments.
-
What is XR, and How is it Transforming Healthcare?
With the global healthcare market for XR estimated to reach $4.6bn in the US alone by 2025, XR is a game-changer for healthcare systems — and there are surprising possibilities for its use in training, recruitment, and beyond!
-
VR Simulation at Johns Hopkins University School of Nursing
As their simulation program expanded, the team at JHU were looking to scale delivery of simulation quickly, using the leading technology and software available. They therefore implemented Oxford Medical Simulation (OMS) Virtual Reality scenarios in pre-licensure and advanced practice programs across the nursing school.
End of content
End of content